
(616) 846-3400
Fax: (616) 846-3406

(616) 846-3400
Fax: (616) 846-3406

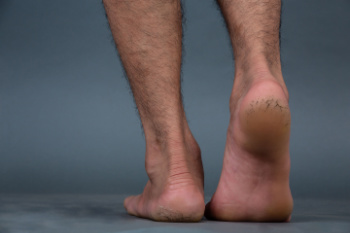 Persistent cracked heels, medically known as heel fissures, can move from a mere cosmetic concern to a painful and potentially serious condition if left untreated. Medical treatment is important for cracked heels that persist for more than a week. A podiatrist, or foot doctor, can remove dead skin to reduce the risk of infection and allow for deeper penetration of therapeutic agents. Podiatrists may also prescribe special creams containing urea or salicylic acid, which are more potent than over-the-counter lotions and designed to hydrate and promote healing in the deeper layers of the skin. In cases where structural issues of the foot contribute to the problem, custom orthotics may be prescribed to redistribute pressure away from the heels. Other possible treatments include bandaging the affected area or using tissue glue to mobilize cracks. If you’re suffering from cracked heels, it is suggested that you make an appointment with a podiatrist to find relief and prevent any complications.
Persistent cracked heels, medically known as heel fissures, can move from a mere cosmetic concern to a painful and potentially serious condition if left untreated. Medical treatment is important for cracked heels that persist for more than a week. A podiatrist, or foot doctor, can remove dead skin to reduce the risk of infection and allow for deeper penetration of therapeutic agents. Podiatrists may also prescribe special creams containing urea or salicylic acid, which are more potent than over-the-counter lotions and designed to hydrate and promote healing in the deeper layers of the skin. In cases where structural issues of the foot contribute to the problem, custom orthotics may be prescribed to redistribute pressure away from the heels. Other possible treatments include bandaging the affected area or using tissue glue to mobilize cracks. If you’re suffering from cracked heels, it is suggested that you make an appointment with a podiatrist to find relief and prevent any complications.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cracked heels can make life very frustrating and embarrassing when displaying the bare feet. Aside from being unpleasing to the eye, they can also tear stockings and socks and wear out shoes at a faster rate. When severe, cracked heels may cause pain or infection.
Cracked heels are a problem for those who are athletic, those who may walk a lot, and those who have especially dry skin. Those who use medication that dry the skin, those who swim often, wearing certain types of shoes, and those who are diabetic may have trouble with cracked heels. Seniors whose skin produces less oil may also have trouble with cracked feet. There is no one way to develop cracked feet, and there is no cure.
Today, the market consists of numerous products that have a variety of ingredients to promote healing. Some of these are over-the-counter. Others are prescribed by a doctor, especially for those who have chronic dry feet and heels.
Some doctors recommend wearing socks at night for those with rough skin. This helps further healing, and helps creams stay on longer and better absorb into the skin.
One way to alleviate dryness that causes cracked heels is by using moisturizers both day and night. Another way is to make sure the skin is clean and dry at all times. Using a pumice stone to buff away dead skin before putting on moisturizer can also help. Cracked heels will not respond to the cream unless the outer layer of skin is first removed through exfoliation. After exfoliation, lotion or ointment will be absorbed by the skin more easily.
Foods that produce healing and balance can also help the skin from within. Everything that is put into the body can either help it or hurt it. Taking supplements of omega-3 fatty acids and zinc can also be very beneficial.
Nevertheless, not all products are guaranteed to help treat cracked feet. Seeing a professional is best if other treatments options were unsuccessful. A podiatrist should be able to give the best advice to help with this problem.
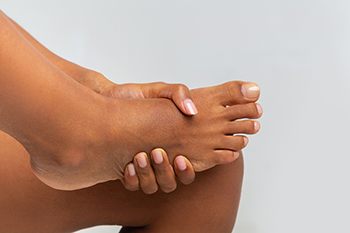
The forefoot consists of various bones, ligaments, tendons, muscles, nerves, and blood vessels, any of which can experience pain. Three main conditions are contributors to forefoot pain. First is metatarsalgia, or discomfort in the ball of the foot. This condition is often triggered by intense athletic training or wearing ill fitting shoes, causing misalignment of bones or spending too much time on the feet. Second, sesamoiditis results from inflammation of tendons that support the two small sesamoid bones, just under the big toe. Inflammation affects weight bearing and inhibits movement of the big toe. Sesamoiditis is common among runners and dancers. Third is Morton’s neuroma, characterized by a thickening of the tissue surrounding the nerves near the toes. This causes burning pain and numbness, and is generally felt between the third and fourth toes. It can worsen by wearing inappropriate footwear or participating in high-impact activities. For advice with any of these painful forefoot ailments, it is suggested that you schedule an appointment with a podiatrist for an accurate diagnosis and tailored treatment plans.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
 The main symptoms of a broken foot are severe pain, swelling, and bruising around the injured area. Some patients may experience very intense pain when touching or applying pressure to the foot. Difficulty or inability to bear weight on the foot, along with visible deformities or changes in foot shape, can also indicate a potential break. Numbness of the foot is another possible symptom. X-rays or other imaging tests are commonly used to confirm the presence of a fracture. Taking immediate steps to address a potential broken foot can lead to a more effective recovery and prevent complications down the line. If you have a painful foot and suspect a break or fracture, it is suggested that you make an appointment with a podiatrist for an accurate diagnosis and appropriate treatment.
The main symptoms of a broken foot are severe pain, swelling, and bruising around the injured area. Some patients may experience very intense pain when touching or applying pressure to the foot. Difficulty or inability to bear weight on the foot, along with visible deformities or changes in foot shape, can also indicate a potential break. Numbness of the foot is another possible symptom. X-rays or other imaging tests are commonly used to confirm the presence of a fracture. Taking immediate steps to address a potential broken foot can lead to a more effective recovery and prevent complications down the line. If you have a painful foot and suspect a break or fracture, it is suggested that you make an appointment with a podiatrist for an accurate diagnosis and appropriate treatment.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Dr. Robbi Young from Grand Haven Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The human foot has 26 different bones, and the foot is divided into three parts: the hindfoot, the midfoot, and the forefoot. Each section of the foot is composed of a different amount of bones. For instance, the forefoot is made up of 19 bones. The midfoot is composed of five smaller bones called the navicular, cuboid, and three cuneiform bones. Lastly, the hindfoot is made up of only the talus and the calcaneus. The feet tend to be vulnerable to slipping and twisting; consequently, fractured bones within the foot are common. When a bone gets crushed, bent, twisted, or stretched it may become broken.
Many foot fractures occur through an accident or trauma. More specifically, common causes for broken feet are car accidents, falls, missteps, or overuse. If you have a broken ankle or foot, you may have one or more of the following symptoms: throbbing pain, swelling, bruising, tenderness, deformities, and difficulty walking.
There are some factors that may put you at a higher risk of developing a broken foot. People who participate in high-impact sports are more likely to develop foot fractures because of the stresses, direct blows, and twisting injuries involved in gameplay. Additionally, those who suddenly increase their activity level are more likely to suffer a stress fracture.
Unfortunately, there are different complications that may arise because of a foot fracture. For instance, arthritis may be caused by fractures that extend into the joints. Bone infections are also possible in open fractures due to the bone being exposed to bacteria. However, there are ways you can help prevent yourself from breaking your foot. One way to avoid fractures is to wear proper footwear. If you plan on going on a run, you should wear running shoes. You should also replace your shoes if you notice that they are becoming worn out. For runners, it is best to replace shoes every 300 to 400 miles.
Treatment for foot fractures usually consists of rest, ice, elevation, and compression (RICE). If you plan on wrapping your foot, try not to wrap it too tightly because doing so may cut off blood supply in the foot. You should also avoid walking on the fractured foot.
If you suspect you have a broken foot, you should see your podiatrist right away. It is important that you have someone bring you to your doctor, since driving with a broken foot can be dangerous. You should especially seek urgent care if you are experiencing numbness, pain, or deformities in your foot.
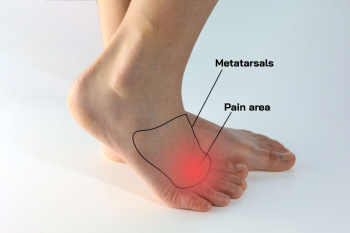
Plantar digital neuroma, also known as Morton's neuroma, is characterized by the thickening of the tissue surrounding the nerves that run between the toes, most often affecting the area between the third and fourth toes. This thickening can cause compression and irritation of the nerve, leading to pain and discomfort. Individuals with plantar digital neuroma typically experience sharp or burning pain in the ball of the foot, tingling or numbness in the toes, and the sensation of standing on a pebble or fold in a sock. Pain may worsen with walking, wearing tight or narrow shoes, or squeezing the forefoot. The discomfort associated with Morton’s neuroma can be disruptive to daily activities and may worsen over time if left untreated. Recognizing the symptoms of plantar digital neuroma is essential for seeking proper diagnosis and treatment to alleviate pain and restore foot health. If you have pain or discomfort between your third and fourth toes, it is suggested that you consult a podiatrist who can confirm Morton's neuroma, and offer correct treatment solutions.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Robbi Young of Grand Haven Foot & Ankle. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
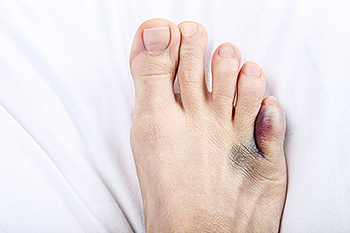
Pain in the pinky toe, though seemingly small, can be a significant source of discomfort, and understanding the potential causes is critical for effective resolution. Wearing ill-fitting footwear emerges as a frequent culprit, as tight shoes or those with narrow toe boxes can compress the pinky toe, leading to friction, irritation, and pain. Stubbing the pinky toe against furniture or other objects is another common cause of acute pain, often accompanied by swelling and bruising. Structural issues such as hammertoes or corns can contribute to ongoing discomfort, creating pressure points on the pinky toe. Additionally, overuse or strain from activities like running or prolonged standing may result in muscle or ligament injuries around the pinky toe. Identifying the specific cause of pinky toe pain is essential for implementing appropriate interventions. If you have pinky toe pain, it is suggested that you consult a podiatrist who can determine what the cause is, and offer appropriate relief and treatment options.
Toe pain can disrupt your daily activities. If you have any concerns, contact Dr. Robbi Young of Grand Haven Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
When to See a Podiatrist
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our office located in Grand Haven, MI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.